Why Medical Claim Rejections Are Surging in 2026 And How Smart Practices Are Stopping Them
Medical claim rejections have always been a challenge for healthcare organizations but in 2026, the problem has intensified. Payers across the U.S. are adopting stricter automation, tighter CMS compliance filters, and more complex prior authorization rules, creating new obstacles for even the most seasoned billing teams. A denial rate of just 10–12% can cost a practice thousands of dollars monthly, reduce cash flow stability, and slow growth. The good news? Most rejections are 100% preventable with the right systems. Let’s break down what’s happening and how high‑performing practices are reversing the trend. By InCareMD Revenue Cycle Experts | +1 (346) 484‑CARE | contact@incaremd.com
3/3/20263 min read


Medical claim rejections have always been a challenge for healthcare organizations but in 2026, the problem has intensified. Payers across the U.S. are adopting stricter automation, tighter CMS compliance filters, and more complex prior authorization rules, creating new obstacles for even the most seasoned billing teams.
A denial rate of just 10–12% can cost a practice thousands of dollars monthly, reduce cash flow stability, and slow growth.
The good news?
Most rejections are 100% preventable with the right systems.
Let’s break down what’s happening and how high‑performing practices are reversing the trend.
What’s Driving the Spike in Claim Rejections in 2026?
InCareMD analysts have identified several forces reshaping the revenue cycle landscape:
Advanced Payer Claim‑Scrubbing Automation
Insurance companies now use AI‑powered scrubbing tools that instantly reject claims with:
coding mismatches
formatting errors
incomplete identifiers
This means even small mistakes cause instant rejection.
Stricter CMS Documentation Requirements
CMS continues tightening standards for ICD‑10‑CM accuracy, modifier use, and medical necessity documentation. Even slight ambiguity can flag a claim.
Expansion of Prior Authorization Requirements
More procedures now require pre‑approval across Medicare Advantage and commercial plans. Missing, expired, or mismatched authorizations trigger automatic denials.
Eligibility Verification Failures
Many rejections still stem from:
inactive coverage
deductible misunderstandings
changes in COB
patient plan switches
Increased Audit and Coding Scrutiny
As payers look for savings, coding accuracy is under the microscope like never before.
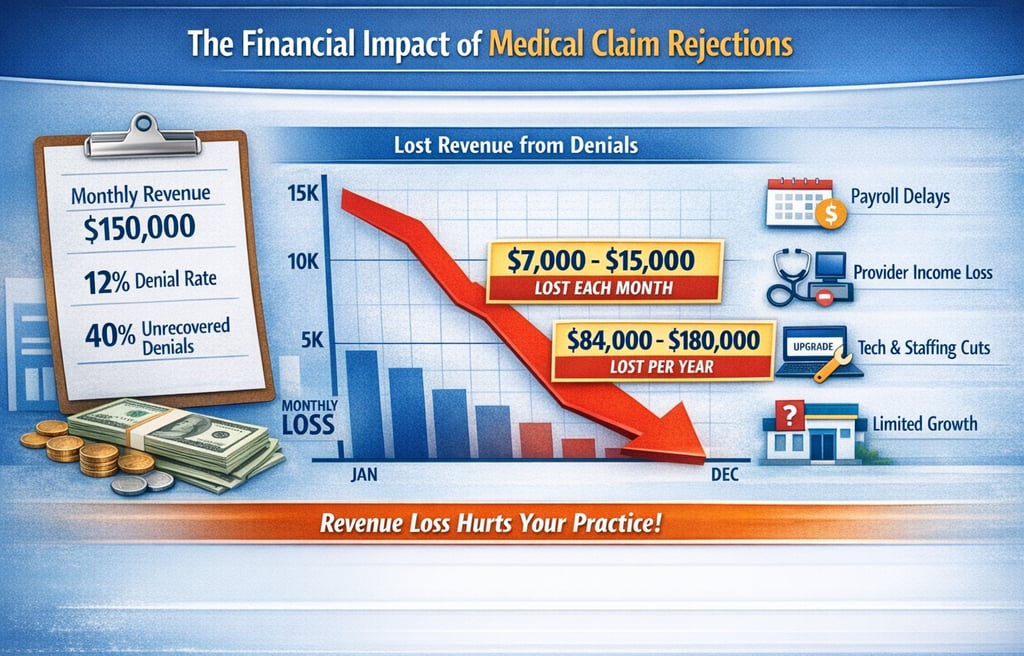
The Financial Impact: What Practices Are Losing Every Month


Let’s look at a real-world example:
Monthly revenue: $150,000
Denial rate: 12%
Unrecovered denials: 40%
Lost revenue per month: $7,000–$15,000
Lost revenue per year: $84,000–$180,000
That’s revenue that could have supported:
payroll
technology upgrades
provider compensation
new staff hiring
patient care expansion
Denial prevention isn’t just a billing task — it’s a financial strategy.
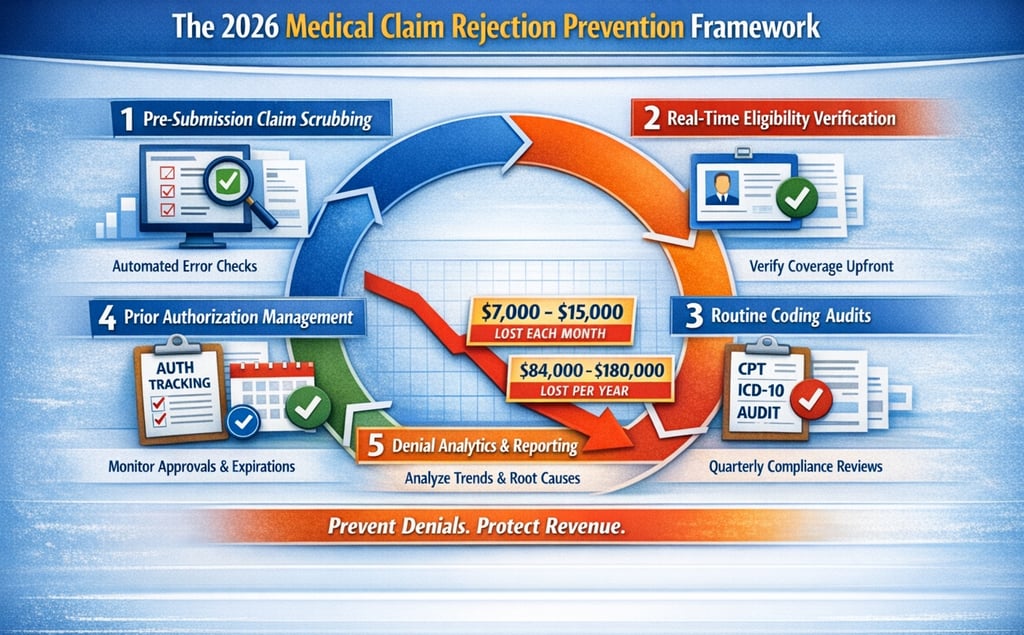
The 2026 Denial Prevention Framework
To stay ahead of increasing rejections, leading healthcare organizations follow a five‑pillar framework:
Pre‑Submission Claim Scrubbing
Automated tools catch:
incomplete codes
demographic errors
NPI mismatches
missing modifiers
medical necessity gaps
before the claim ever reaches the payer.
Real‑Time Eligibility Verification
Eligibility should be checked:
before the appointment
at check‑in
before claim submission (for high‑risk payers)
This eliminates the #1 root cause of denials.
Quarterly Coding Compliance Audits
Regular audits reveal:
incorrect CPT® / ICD‑10‑CM use
unsupported diagnoses
insufficient documentation
undercoding and overcoding risks
Prior Authorization Tracking
Practices need:
a centralized dashboard
expiration reminders
linked diagnosis codes
payer‑specific rules
A structured workflow cuts PA‑related denials by up to 40%.
Denial Analytics & Root‑Cause Reporting
Monitoring CARC/RARC trends helps identify systemic problems like:
recurring coding errors
staff training needs
payer-specific rejection patterns
Analytics transform denial management from reactive → proactive.
Is Your Practice at Risk?
Use this quick self-check:
✔ Do you track denial rates monthly?
✔ Do you analyze CARC/RARC codes?
✔ Is eligibility verified every visit?
✔ Do you run quarterly coding audits?
✔ Is prior authorization fully tracked?
✔ Is your clean-claim rate above 95%?
If you answered “No” to two or more, your revenue cycle may be leaking money.
Complimentary Revenue Health Check

InCareMD offers a free, no‑obligation assessment to identify hidden revenue risks and streamline your billing process.
Includes:
✔ Denial Rate Analysis
✔ Coding Risk Review
✔ Eligibility Workflow Assessment
✔ Prior Authorization Audit
✔ AR Performance Snapshot
📞 +1 (346) 484‑CARE
📧 contact@incaremd.com
InCareMD (Strengthening the Financial Heart of Your Practice.)


